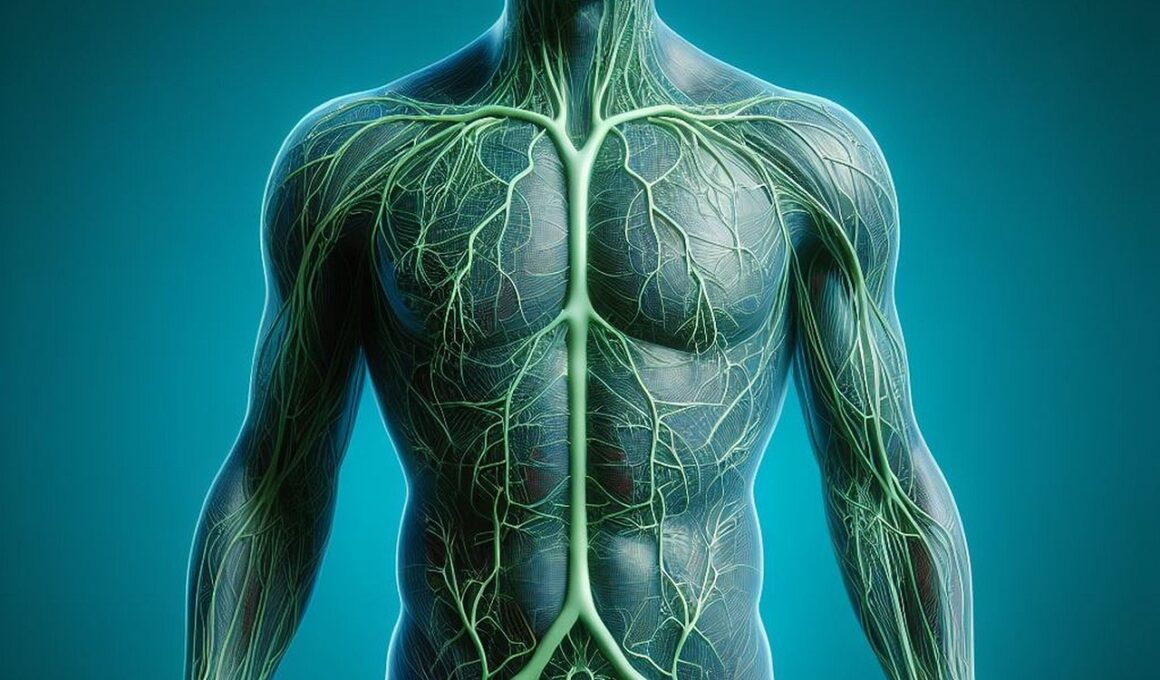
Infection Prevention Strategies for Lymphedema Patients
Maintaining proper hygiene is crucial for patients suffering from lymphedema. Keeping the affected areas clean and dry can significantly reduce infection risks. Patients should wash their skin daily using mild soap and warm water. After washing, it is essential to gently pat the skin dry, avoiding any vigorous rubbing. Additionally, moisturizers should be applied regularly to prevent dryness and cracking of the skin. Health professionals recommend avoiding excessive moisture and friction during daily activities. Potential sources of trauma, such as insect bites or cuts, must be treated promptly. In case of any injury, disinfect the area immediately to prevent bacteria from entering. Furthermore, utilizing protective gloves when gardening or cleaning is advisable to prevent injuries. Always keep nails trimmed short and smooth to minimize the chances of skin tears, especially around sensitive areas. Wearing appropriate, breathable clothing can also help protect from skin irritations. For optimal health, patients should routinely monitor their skin for any signs of redness, swelling, or unusual drainage. Early detection allows for prompt treatment before minor issues escalate into significant infections.
One effective infection prevention strategy includes immunizations. Ensuring that lymphedema patients are up-to-date on vaccinations is vital for reducing infection risks. Vaccines protect against illnesses that could lead to complications. For example, the flu vaccination is crucial since flu symptoms can exacerbate existing lymphedema. Another important vaccine is the pneumococcal vaccine, which helps shield against pneumonia and other serious respiratory infections. Additionally, engaging in regular health check-ups provides an opportunity for early detection of potential health issues. During these visits, patients can discuss any concerns related to their lymphedema management. Health care professionals may recommend personalized strategies tailored to individual needs, improving overall infection control. Patients should also be educated about signs of infections, such as increased swelling, warmth, or discharge from the affected limb. Awareness empowers individuals to seek timely medical intervention, preventing further complications or hospitalizations. Furthermore, support groups or educational workshops can help patients connect with others experiencing similar challenges. These platforms provide valuable advice on coping strategies and share personal experiences that can enhance infection prevention methods.
Daily Care Regimens
In addition to skin care practices, patients should establish thorough daily regimens to enhance lymphedema management. Regular exercise, combined with proper skin care, plays a crucial role in maintaining lymphatic health. Gentle exercises such as walking, swimming, or yoga can stimulate lymphatic circulation and minimize swelling. Always consult with a physical therapist or healthcare provider before starting new exercises to ensure safety. Compression garments are another essential component for managing lymphedema. These garments must fit well to help maintain appropriate pressure, reducing swelling effectively. It’s important to wear them during the day and remove them at night unless advised otherwise by a healthcare professional. Additionally, maintaining a healthy diet supports immune function. A balanced diet rich in vitamins, minerals, and antioxidants promotes healing and supports overall health. Staying adequately hydrated is equally important, as fluids help transport nutrients throughout the body, vital for healing and recovery. Furthermore, resting regularly allows individuals to manage fatigue, especially during flare-ups. This balance of activity, rest, and nutrients is vital for patients aiming to minimize the risk of infections related to lymphedema.
Patients should recognize environmental factors that may contribute to infection risks. Extreme temperatures can exacerbate swelling, so maintaining a stable environment is essential. During hot weather, patients must stay cool and avoid prolonged sun exposure, as heat can lead to increased perspiration and bacterial growth. Similarly, in cold conditions, proper clothing layers help retain body heat and minimize exposure to icy elements that may damage skin integrity. Humidity plays a significant role as well, as excessive moisture promotes fungal infections. Applying antifungal powders may help in more humid environments. Avoiding contact with potential irritants, such as harsh chemicals or dyes, can protect delicate skin. Choosing gentle household products and natural fabrics can make a noticeable difference in comfort. Patients must be vigilant when selecting personal care products, ensuring they are free from irritating ingredients. Stress management techniques are also important, as high-stress levels can weaken the immune system. Engaging in relaxation activities, such as meditation or mindfulness exercises, can assist in reducing stress and improving overall health. Managing these environmental aspects contributes significantly to lymphedema patients’ overall infection prevention strategies.
Collaborating with Healthcare Providers
Building a comprehensive support system is vital for effective lymphedema management. Collaborating with healthcare providers, including doctors, physical therapists, and dietitians, can enhance patient outcomes. Regular follow-ups with healthcare professionals allow for personalized adjustments to treatment plans. These experts can recommend individualized strategies to prevent infections based on specific needs and circumstances. Patients should feel encouraged to ask questions during appointments, clarifying any doubts regarding their treatment. This dialogue fosters trust and ensures proper interventions are made. Incorporating care support layers, such as family and friends, also contributes significantly to a robust support network. Loved ones can provide encouragement and assistance with daily routines, creating a motivating environment. Peer support groups allow patients to share experiences and learn from each other’s coping mechanisms. Additionally, healthcare teams should act proactively by educating patients about potential complications of lymphedema. This knowledge equips patients to identify early warning signs of infections or other issues, prompting immediate medical attention. By taking a proactive approach, patients enhance their infection prevention strategies and improve overall well-being.
While lymphedema poses significant challenges, patients can adopt numerous strategies to minimize infection risks. Educating oneself and employing consistent self-care practices ultimately enhance individual health outcomes. Simple practices such as frequent handwashing, not sharing personal items, and being cautious about outdoor activities are essential. For instance, avoiding barefoot walking can protect against cuts and scrapes that lead to infections. Furthermore, wearing sunscreen on exposed skin can help prevent sunburns, which serves as potential gateways for bacteria. Adequate hydration is crucial as well, as it supports skin, lymphatic fluid movement, and overall health. Hence, patients should strive to drink plenty of water to support their bodies. Another effective tip is incorporating immune-boosting foods, such as garlic, ginger, or turmeric, which possess antimicrobial properties. Including these foods can potentially enhance the immune response. Moreover, regular communication with healthcare providers can yield accountability, ensuring patients adhere to preventive measures. Lifestyle adjustments, when implemented consistently, play a crucial role in infection prevention. Lymphedema patients can confidently reduce their risks and improve their quality of life by focusing on proactive health management.
Conclusion
Finally, developing a comprehensive infection prevention strategy tailored specifically for lymphedema patients is paramount. By implementing the outlined practices and collaborating effectively with healthcare providers, individuals can manage their condition with assurance and confidence. Awareness about infection risks associated with lymphedema is essential. This understanding allows patients to make informed decisions regarding their health. Comprehensive education on lifestyle adjustments can promote a strong sense of agency over their health outcomes. Enhanced communication between patients and healthcare providers fosters a supportive environment that contributes immensely to effective recovery modalities. As lymphedema management progresses, patients should be adaptable and open to changing needs. Engaging with healthcare professionals facilitates ongoing monitoring and assurance that strategies remain effective. Ultimately, infection prevention is integral to lymphedema management. By prioritizing these strategies, patients can enjoy a better quality of life, reduced complications, and greater emotional well-being. The journey might be challenging, but empowered individuals equipped with effective strategies can navigate their health with confidence. Ongoing education, support, and commitment to self-care will guide patients toward optimal health and well-being.
Utilizing the appropriate resources like informational articles on lymphedema can be beneficial. By understanding their condition better, patients can implement effective infection prevention strategies. Collaborating with support systems enhances emotional health during this journey. With diligent efforts and awareness, lymphedema patients can significantly reduce infection risks, leading to a more fulfilling life.