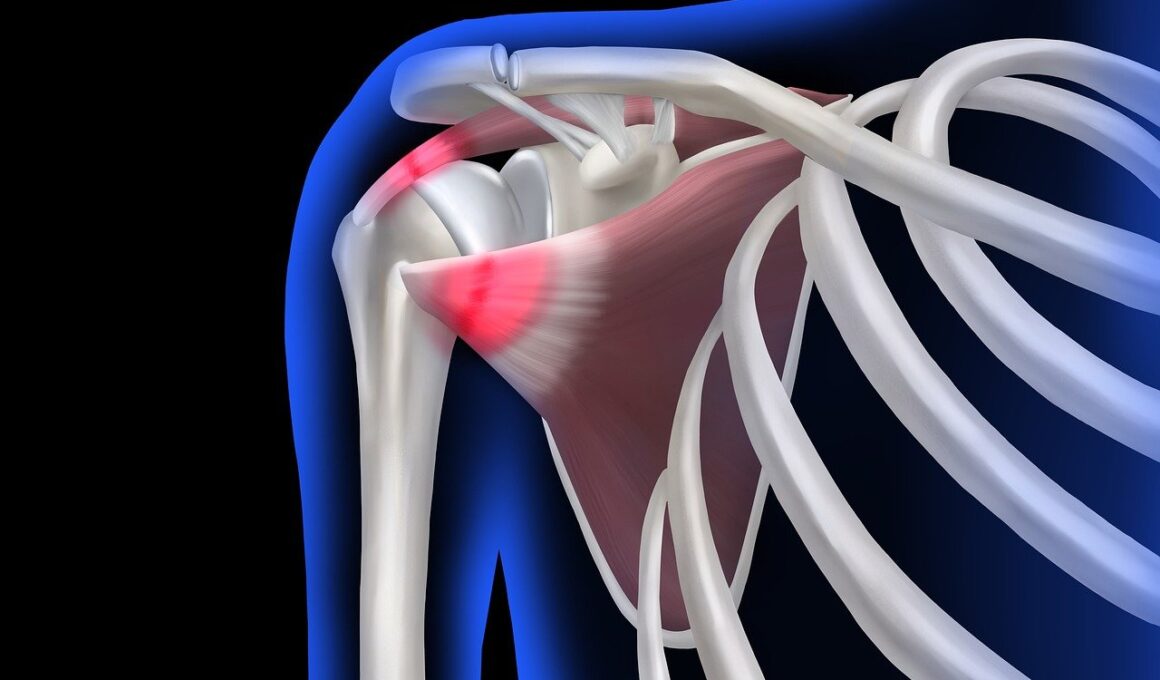
Functional Movement Training for Chronic Shoulder Impingement Syndrome
Functional Movement Training (FMT) is an essential method for addressing chronic conditions like Shoulder Impingement Syndrome (SIS). Individuals suffering from SIS often experience discomfort and limitations in shoulder mobility, impacting daily life profoundly. The goal of FMT is to improve both functional movement patterns and strength, facilitating recovery and preventing further injuries. This training emphasizes body awareness, joint stabilization, and muscular balance. By evaluating movement deficiencies, clinicians can tailor necessary interventions that directly target the underlying issues causing pain. During FMT, special attention is given to proper alignment and the integration of movements that mimic daily activities, ensuring that rehabilitation becomes relevant to each patient’s lifestyle. These principles not only aim to relieve pain but also work towards restoring individuals’ abilities to perform tasks they enjoy. Additionally, FMT can enhance coordination and strength in supporting muscles, mitigating the chances of re-injury. Ultimately, employing functional movement strategies can significantly improve life quality for those with Chronic Shoulder Impingement Syndrome, leading to a more active and fulfilling life.
Understanding the anatomical basis of SIS is crucial to successful intervention strategies. The shoulder joint’s anatomy involves dynamic interactions among bones, muscles, tendons, and ligaments. Shoulder impingement typically occurs when the rotator cuff tendons become inflamed or injured, often due to repetitive overhead motions. These tendons can become compressed during shoulder elevation, resulting in painful sensations and restricted mobility. Therefore, recognizing scapular mechanics plays a vital role in alleviating symptoms associated with SIS. A strong and well-coordinated scapula stabilizes the shoulder joint, allowing for optimal movement and reducing impingement risk. During FMT, exercises focusing on scapular upward rotation and external rotation strengthen the surrounding musculature. Incorporating serratus anterior and lower trapezius strengthening exercises helps improve scapular control during shoulder movements. Research indicates that targeting these specific muscle groups can significantly reduce discomfort and increase joint function. Moreover, integrating manual therapy techniques may enhance the efficacy of FMT, enabling faster returns to sport and daily activities. Hence, understanding the body’s structural intricacies is essential for developing effective FMT protocols for individuals suffering from chronic shoulder problems.
Assessment and Evaluation Techniques
Before implementing any therapeutic exercise programs for chronic shoulder impingement, a comprehensive assessment is critical. Evaluations encompass evaluating range of motion (ROM), strength, and functional capabilities. Several standardized assessment tools can facilitate this process, including the Oxford Shoulder Score and Disabilities of the Arm, Shoulder, and Hand (DASH) questionnaire. These tools not only provide insight into physical limitations but also help identify patients’ specific goals and expectations. A thorough assessment helps detect compensatory movement patterns that may worsen shoulder symptoms, allowing therapists to develop individualized strategies. This thorough evaluation process also informs decision-making when setting appropriate exercise intensities and progressions. While assessing physical capabilities, subjective complaints should not be overlooked. Open communication about pain experiences during daily activities can significantly highlight specific functional limitations. Regularly re-assessing functional movement abilities throughout the treatment program allows professionals to modify exercise plans, ensuring continued effectiveness. This iterative evaluation approach enhances communication between therapists and patients while promoting adherence to rehabilitation goals. Thus, the assessment in FMT forms a bedrock for personalized intervention, optimizing outcomes for SIS management.
Progressive exercise interventions represent a cornerstone for the effective management of shoulder impingement syndromes. Initiating a program with simple range-of-motion exercises is advisable to gradually improve flexibility, progressively moving to strengthening and stabilization exercises. Incorporates dynamic stability drills that challenge shoulder joint integrity during functional tasks. Examples include wall slides, shoulder circles, and pendulum swings. Once patients demonstrate adequate mobility, increasing resistance through light weights or resistance bands facilitates further enhancement of muscular strength. Exercises targeting the rotator cuff muscles, such as external rotations and internal rotations, contribute to joint stabilization and pain reduction. Moreover, integrating multi-directional movements mimics everyday activities, encouraging functional adaptability. This multifaceted approach to shoulder rehabilitation also includes balance-based training, which can improve proprioception—the body’s awareness of joint position and movement. Research supports the use of progressive resistance exercises for SIS rehabilitation, indicating improved functional outcomes and pain reduction. Therefore, sequencing exercises strategically while monitoring patient feedback allows for a streamlined rehabilitation pathway, promoting optimal shoulder recovery. Consistency and patience are critical, as progress may take time, but maintaining motivation through regular evaluations fosters engagement and determination.
Functional Movement Patterns
Adopting functional movement patterns can yield beneficial results in patients with SIS. These patterns allow the body to perform tasks naturally and efficiently, reflecting real-life activities. Functional movements such as reaching, lifting, and throwing are essential for restoring lost capabilities. Training that emphasizes these activities encourages the body to reorganize itself for optimal movement efficiency. When patients engage in these functional patterns, they can restore proper alignment, thereby alleviating pain. Techniques like kinetic chain training, which promote simultaneous engagement of multiple muscle groups, should form part of an effective regimen. Additionally, employing the concept of closed kinetic chain exercises enhances joint stability and reduces shear forces on the shoulder. Exercises such as wall push-ups and shoulder taps shift the focus from isolated muscle actions to collaborative movements. Also, ensuring proper activation of core muscles supports the shoulder girdle, further enhancing the functional synergy between upper and lower extremities. Clinical evidence highlights improved outcomes for shoulder impingement conditions resulting from functional training methodologies. Hence, incorporating functional movement patterns within the training regimen optimizes rehabilitation effectiveness for those suffering from SIS.
Education plays a vital role in managing chronic shoulder conditions, and it is essential to empower patients through understanding. Therapists should provide comprehensive information regarding SIS, enhancing awareness of contributing factors and encouraging active participation. Educating patients about avoiding postures that exacerbate symptoms, such as repetitive overhead activities or poor ergonomics, can greatly influence their recovery trajectory. Additionally, motivating patients to adopt healthy lifestyle changes can substantially diminish chronic pain risks. Topics like weight management, ergonomic workstation setups, and strategies for maintaining good posture are invaluable. Furthermore, exposing patients to injury prevention practices, such as warm-up routines and proper lifting techniques, fosters a proactive approach to self-care. Encouragement to apply these concepts outside therapy sessions reinforces the commitment to their health journey. Following up regularly to assess understanding creates an open dialogue, allowing team members to adapt educational interventions accordingly. Consequently, emphasizing education while engaging in FMT supports sustainable behavior change, aids adherence to prescribed exercises, and ultimately fosters long-term recovery. Empowered patients are better equipped to manage their conditions and lead healthy lives, aligning with the primary goals of rehabilitation.
Conclusion
Functional Movement Training provides a comprehensive framework for rehabilitating chronic shoulder impingement syndromes effectively. The integration of evidence-based practices, personalized assessments, and progressive interventions optimizes recovery outcomes. Through understanding shoulder anatomy and functional deficits, individualized programs can address specific movement patterns, promoting long-term health. The focus on education and patient empowerment furthers the effectiveness of rehabilitation efforts. Developing a supportive therapeutic relationship encourages engagement and motivation, key elements in navigating the recovery process. As patients learn about their condition’s nature, they become active participants in their healing journey. The emphasis on functional movement patterns ensures that exercises are relevant to individual lifestyles, enabling patients to return to their daily activities confidently. Moreover, recognizing the significance of enhancing overall musculoskeletal health through retraining promotes resilience against potential future injuries, ensuring a better quality of life. In conclusion, Functional Movement Training is pivotal in managing chronic conditions like Shoulder Impingement Syndrome, providing strategies for pain relief, increased mobility, and improved everyday function, ultimately enhancing life quality and fulfilling a socially active lifestyle.