Evaluating Cardiac Output Changes Post-Exercise Using Imaging Technologies
Cardiac output is a crucial parameter in assessing cardiovascular health, especially following exercise. Various imaging technologies have evolved to measure this parameter accurately. Echocardiography, for instance, offers real-time visualization of the heart’s function and hemodynamics. It provides insight into the heart’s efficiency in pumping blood during physical exertion. Cardiac MRI is another advanced imaging modality that allows non-invasive assessment of heart structure and blood flow. It excels in capturing detailed information about cardiac muscles and chambers under various conditions. Nuclear imaging techniques, such as PET and SPECT, can evaluate myocardial perfusion and oxygen consumption during stress testing. Each technique has unique advantages and limitations. Thus, a comprehensive approach is essential to selecting the right imaging method for evaluating cardiac output changes post-exercise. Accurate assessment helps guide treatment strategies and improve patient outcomes. Additionally, understanding the biomechanics of the heart under stress can unveil hidden cardiovascular risks that might not be apparent at rest. With continuous advancements in imaging technology, there is hope for heightened precision in cardiac evaluations, leading to more effective interventions and better patient management outcomes.
The Role of Imaging Techniques in Cardiac Assessment
When evaluating cardiac output, the role of imaging techniques becomes paramount, as each provides unique insights. Echocardiograms, for instance, utilize sound waves to create heart images, allowing real-time assessments. This technique is helpful during stress testing to identify how the heart responds under physical conditions. Meanwhile, Cardiac MRI offers a detailed, high-resolution view of cardiovascular structures, enabling precise measurement of volumes and function. This is particularly beneficial for patients with complex anatomical variations. Nuclear imaging techniques, such as PET scans, specifically measure blood flow distribution, illuminating areas with inadequate perfusion. The choice of imaging modality significantly impacts assessment accuracy. Clinicians must consider various factors, including patient history, presentation, and specific exercise protocols. For example, patients with recent myocardial infarctions may require careful imaging to avoid complications. Each technique also varies in sensitivity to exercise-induced changes, making the choice of imaging crucial for accurate assessments. Ultimately, a multifaceted strategy, combining different modalities, may yield more comprehensive evaluations of cardiac dynamics post-exercise. This integrated approach underscores the necessity for ongoing research and development in cardiac imaging technology.
Effective communication plays a vital role in using imaging technologies for cardiac assessment. Clinicians must explain the purpose and process of tests to patients to alleviate concerns and ensure cooperation. Patients often possess varying levels of understanding about imaging techniques and their significance in gauging heart health. Therefore, education can be beneficial, helping to set realistic expectations regarding results and the implications of findings. Moreover, involving patients in discussions about their treatment plans encourages adherence to prescribed exercise regimens, ultimately enhancing cardiac output post-exercise. Coordinating care through multidisciplinary teams can also improve patient outcomes. This ensures that cardiologists, imaging specialists, and physical trainers collaborate effectively. Accountability and transparency across all professionals involved are essential for successful evaluations. Furthermore, it is crucial to monitor patients post-exercise to evaluate the efficacy of prescribed therapies. Regular follow-ups and adjustments can optimize results and encourage long-term health. By prioritizing clear communication, a supportive environment promotes better patient compliance. In turn, this leads to enhanced assessments of cardiac function, shaping strategies aimed at improving overall cardiovascular health.
Understanding the Physiological Responses during Exercise
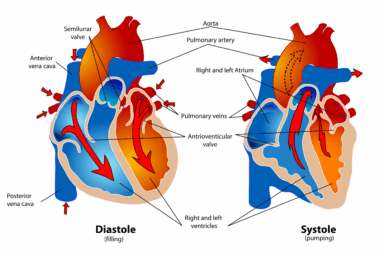
Understanding the physiological responses that occur during exercise is paramount for evaluating cardiac output accurately. The body undergoes numerous adaptations, requiring immediate cardiac adjustments. During intense exercise, the heart rate increases significantly, enhancing blood flow to essential organs and musculature. Additionally, stroke volume, or the amount of blood ejected per heartbeat, also rises, influenced by increased venous return and contractility. Cardiac output is the product of heart rate and stroke volume, and effective imaging techniques can capture these dynamic changes. By utilizing echocardiography or Cardiac MRI, clinicians can visualize these adaptations in real-time. This direct observation assists in determining how well the heart copes with the demands of exercise, thereby identifying possible underlying health issues. Furthermore, accurate assessments can aid in designing tailored exercise programs, focusing on areas that enhance overall cardiovascular health. A thorough understanding of exercise physiology translates to more effective management strategies for individuals, especially those with pre-existing cardiac conditions. Identifying safe parameters for exercise can guide rehabilitation programs, ultimately supporting patients in achieving their health goals.
Recent studies emphasize the importance of evaluating cardiac output through established protocols, ensuring robust data collection. Consistent test environments and standardized exercise regimens yield reliable results. This becomes crucial when comparing patient outcomes: before and after exercise through varied imaging modalities. Whether using stress echocardiography, where ultrasound is employed in conjunction with exercise, or observing changes through MRI scans, a systematic approach is key. Furthermore, rapid technological advancements enable improved imaging resolution, helping clinicians assess changes in cardiac function quickly and effectively. Recent innovations include advanced Doppler imaging to analyze flow dynamics. Additionally, automated software programs can streamline the analysis of changes in cardiac output. These developments necessitate ongoing training for healthcare professionals, ensuring they remain adept in using such innovative tools. Continuous education is vital in interpreting imaging results accurately, leading to better-informed clinical decisions. Moreover, integrating findings from various imaging techniques can enhance understanding, leading to personalized treatment plans. Research reflects a compelling need for comprehensive evaluations to assist clinicians and patients in navigating the nuances of cardiac health management successfully.
Future Directions in Cardiac Imaging Technology
Looking ahead, the future of cardiac imaging technology is promising, bringing innovations to traditional methodologies. Advancements in artificial intelligence (AI) are anticipated to revolutionize how imaging assessments are performed. AI can assist by automating image analysis, enabling real-time, precise evaluations. This shift could reduce human error and improve the accuracy of cardiac output measurements. Furthermore, integrating machine learning algorithms will allow for predictive modeling of cardiac responses during varying exercise intensities. As imaging technologies evolve, the combination of data from different modalities can enhance diagnostic accuracy. Innovative tools, such as wearable sensors, for example, can monitor real-time heart performance during exercise. This information can feed into imaging technologies, providing a comprehensive overview of cardiac health. Furthermore, developments in 3D imaging will improve visualization, leading to enhanced surgical planning and intervention strategies. Ultimately, a shift towards personalized medicine can facilitate tailored treatment approaches based on individual cardiac metrics. Continuous research in this area is crucial to stay abreast of changes driving advancements in technology and diagnostics, ultimately benefiting patients through enhanced healthcare delivery.
In conclusion, the evolution of cardiac imaging technologies provides unprecedented opportunities to evaluate cardiac output following exercise. These modalities enable healthcare practitioners to visualize, measure, and understand the physiological responses exerted during physical activity comprehensively. The integration of various imaging techniques supports accurate assessments, ultimately guiding therapeutic strategies tailored to patients’ individual needs. Fostering collaborations between imaging specialists, cardiologists, and exercise physiologists strengthens care continuity and enhances overall treatment efficacy. As new methodologies continue to emerge, so will the potential to improve diagnostic accuracy and patient outcomes. Patient education and engagement remain integral to this process, ensuring compliance and commitment to prescribed interventions. The trajectory of research in this field remains promising, highlighting the critical role imaging technologies play in not just cardiac assessment but in understanding the complexities of heart health. Continuous improvements and innovations are vital for optimizing cardiac care and rehabilitation approaches. Emphasizing the significance of accurate evaluations and robust data will lead to better health outcomes for patients. The future of cardiac output assessment remains bright as we embrace advancements accelerating our understanding of cardiovascular dynamics.
Implementing these state-of-the-art techniques will ultimately require a commitment to continuous training and professional development within the healthcare community. Understanding the unique characteristics of each imaging modality is crucial for clinicians. However, this must be complemented by effective communication with patients about test procedures and what to expect during assessments. An informed patient is less anxious and more likely to engage fully during evaluations, leading to better data collection. Moreover, healthcare providers should foster a culture of teamwork, bridging the gap between medical imaging specialists and cardiologists, making every interaction more efficient and valuable. Future advancements should also explore user-friendly imaging interfaces, improving usability for clinicians and minimizing patient discomfort. As innovative technology becomes more accessible, it opens the door for a broader patient population to benefit from cardiac imaging evaluations. Furthermore, the integration of telehealth can revolutionize follow-up care, allowing remote assessments and consultations, thereby enhancing accessibility to advanced cardiac care services. The future landscape of cardiac output measurement will thrive on the synergy between emerging technologies and compassionate patient-centered care.